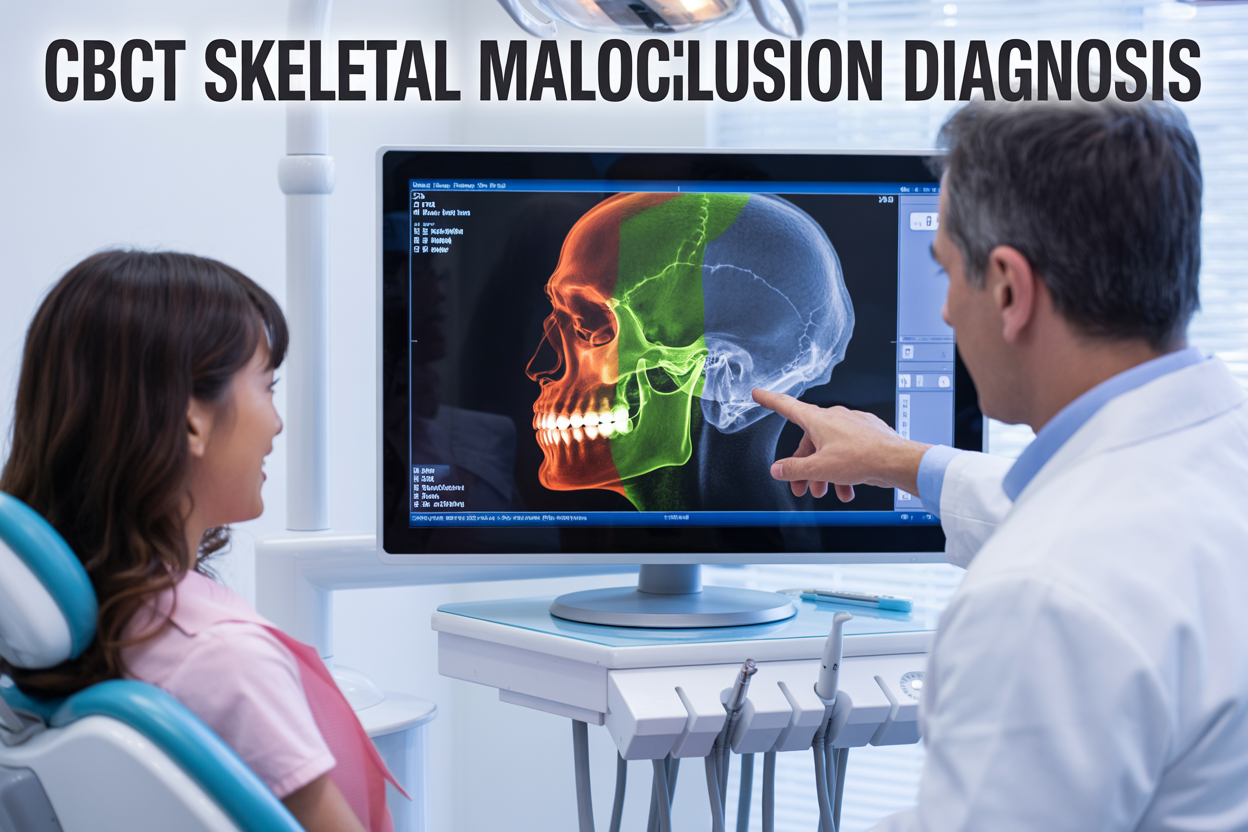
CBCT orthodontics has changed how dental professionals approach skeletal malocclusion diagnosis, moving beyond traditional 2D imaging to provide detailed 3D views of jaw structures and facial bones. This advanced cone beam computed tomography technology gives orthodontists, oral surgeons, and general dentists the precise anatomical information needed to identify complex skeletal patterns that standard X-rays often miss.
For orthodontic practitioners looking to improve diagnostic accuracy and treatment outcomes, understanding CBCT applications can make the difference between good and exceptional patient care. The technology excels at revealing skeletal Class II malocclusion patterns, asymmetries, and other structural issues that impact treatment planning decisions.
This guide covers three key areas: how CBCT cephalometric analysis provides superior diagnostic capabilities compared to traditional methods, the specific ways 3D dental imaging helps identify different skeletal malocclusion patterns, and practical strategies for CBCT treatment planning that lead to more predictable orthodontic results. You’ll learn when this orthodontic imaging technology offers the most value and how to integrate these diagnostic tools into your clinical workflow effectively.
Understanding CBCT Technology for Orthodontic Applications
Three-dimensional imaging capabilities versus traditional radiography
CBCT orthodontics revolutionizes how practitioners visualize and diagnose skeletal malocclusion by providing comprehensive 3D dental imaging that traditional two-dimensional radiographs simply cannot match. While conventional cephalometric radiographs offer only lateral and frontal views with inherent magnification and distortion, cone beam computed tomography captures the entire craniofacial complex in true three-dimensional detail.
Traditional radiography forces orthodontists to mentally reconstruct spatial relationships from flat images, often missing critical anatomical variations. CBCT technology eliminates this guesswork by presenting actual volumetric data where practitioners can examine structures from any angle, measure distances accurately, and identify asymmetries that might remain hidden in conventional films.
The technology proves particularly valuable when diagnosing complex skeletal Class II malocclusion cases where multiple planes of space require evaluation. Practitioners can assess TMJ positioning, airway dimensions, and root-to-cortical bone relationships simultaneously, creating a complete diagnostic picture that supports more precise treatment decisions.
| Imaging Method | Dimensional View | Anatomical Detail | Measurement Accuracy |
|---|---|---|---|
| Traditional Ceph | 2D lateral/frontal | Limited overlap resolution | ±5-10% magnification error |
| CBCT | True 3D volumetric | Complete anatomical clarity | <1% measurement error |
Radiation exposure considerations and safety protocols
Modern CBCT systems deliver significantly lower radiation doses compared to medical CT scanners while maintaining diagnostic quality for orthodontic applications. Recent technological advances have reduced effective radiation doses to levels comparable with a full-mouth series of traditional dental radiographs.
Patient safety remains paramount when implementing orthodontic imaging protocols. Current CBCT units employ pulsed exposure techniques and advanced filtering systems that minimize radiation while optimizing image quality for skeletal malocclusion diagnosis. Most orthodontic CBCT scans require exposure times of only 10-40 seconds with effective doses ranging from 50-200 microsieverts.
Practitioners must follow ALARA principles (As Low As Reasonably Achievable) by:
- Selecting appropriate field of view sizes for specific diagnostic needs
- Using child-specific protocols for pediatric patients
- Implementing proper patient positioning and stabilization
- Regular equipment calibration and maintenance schedules
Age-specific considerations become critical since younger patients show higher radiation sensitivity. Orthodontists should justify CBCT use based on diagnostic necessity rather than routine screening, particularly when treating developing patients with skeletal growth remaining.
Image resolution and diagnostic accuracy improvements
CBCT cephalometric analysis offers submillimeter resolution capabilities that dramatically enhance diagnostic precision for complex malocclusion cases. Modern systems achieve voxel sizes as small as 0.125mm, allowing detailed examination of anatomical structures that traditional radiography cannot adequately visualize.
This enhanced resolution proves crucial when evaluating:
- Precise condylar positioning and TMJ morphology
- Root proximity to vital structures during treatment planning
- Alveolar bone thickness for anchorage considerations
- Airway dimensions and their relationship to skeletal patterns
Diagnostic accuracy improvements become most apparent in cases involving facial asymmetries, impacted teeth, or unusual anatomical variations. The technology enables practitioners to measure angular and linear relationships with unprecedented precision, reducing diagnostic uncertainty that often complicates traditional cephalometric interpretation.
Three-dimensional reconstruction capabilities allow for virtual treatment simulations where orthodontists can predict outcomes more reliably. Software advances enable automatic landmark identification and measurement protocols that standardize CBCT treatment planning across different practitioners and clinical settings.
Cost-effectiveness in complex malocclusion cases
CBCT technology demonstrates clear economic advantages when managing complex orthodontic cases that would otherwise require multiple diagnostic procedures and potential treatment revisions. While initial imaging costs exceed traditional radiography, the comprehensive diagnostic information often prevents costly treatment complications and reduces overall therapy duration.
Complex skeletal malocclusion cases benefit most from CBCT investment through:
- Reduced need for multiple conventional radiographs throughout treatment
- Earlier identification of anatomical limitations that affect treatment outcomes
- More accurate treatment time predictions leading to better practice scheduling
- Decreased liability risks through comprehensive documentation
The technology proves particularly cost-effective for surgical orthodontic cases where precise measurements directly impact surgical planning accuracy. Many practices report that improved diagnostic confidence leads to more predictable treatment outcomes and higher patient satisfaction rates.
Insurance coverage for CBCT continues expanding as evidence supporting its diagnostic value grows. Many carriers now approve CBCT imaging for specific indications including impacted teeth, TMJ disorders, and complex skeletal discrepancies that require three-dimensional evaluation for optimal treatment planning.
Return on investment calculations show that practices handling moderate volumes of complex cases typically recover CBCT equipment costs within 18-24 months through improved case acceptance rates and reduced treatment complications.
Identifying Skeletal Malocclusion Patterns with CBCT
Class I, II, and III Skeletal Discrepancies Detection
CBCT orthodontics transforms how we identify and analyze skeletal malocclusion patterns by providing three-dimensional visualization of craniofacial structures. Unlike traditional lateral cephalograms, cone beam computed tomography delivers precise measurements of the maxilla, mandible, and their relationship to the cranial base.
Class II skeletal malocclusion detection through CBCT reveals anteroposterior jaw discrepancies with remarkable accuracy. The technology allows orthodontists to measure ANB angles, Wits appraisal, and evaluate the actual position of the maxilla and mandible in three dimensions. CBCT cephalometric analysis shows whether the skeletal Class II pattern stems from maxillary protrusion, mandibular retrusion, or a combination of both factors.
Class III skeletal patterns become clearly visible through CBCT imaging, particularly when evaluating the mandibular prognathism or maxillary deficiency. The detailed bone architecture visualization helps distinguish between dental compensations and true skeletal discrepancies, which proves essential for treatment planning decisions.
| Skeletal Class | ANB Angle | Key CBCT Features |
|---|---|---|
| Class I | 2-4° | Balanced jaw relationship |
| Class II | >4° | Maxillary prominence or mandibular retrusion |
| Class III | <2° | Mandibular prominence or maxillary deficiency |
CBCT orthodontic diagnosis also reveals vertical skeletal patterns that affect facial harmony and dental function. The technology provides accurate measurements of facial heights, mandibular plane angles, and helps identify high-angle or low-angle growth patterns that significantly impact treatment approaches.
Asymmetrical Facial Growth Pattern Analysis
Facial asymmetries present complex diagnostic challenges that CBCT technology addresses with exceptional precision. Skeletal malocclusion diagnosis through three-dimensional imaging reveals subtle asymmetries that traditional two-dimensional radiographs often miss or misrepresent.
CBCT orthodontics enables comprehensive evaluation of mandibular asymmetries by measuring chin point deviation, condylar height differences, and ramus length variations. The technology provides accurate measurements of how the mandible relates to the midsagittal plane, helping orthodontists distinguish between functional shifts and true skeletal asymmetries.
Maxillary asymmetries become apparent through CBCT analysis of the maxillary complex, including the alveolar process, maxillary sinus development, and nasal cavity structure. These asymmetries often correlate with unilateral crossbites or dental midline discrepancies that require specific treatment approaches.
The power of 3D dental imaging lies in its ability to quantify asymmetries with millimeter precision. Orthodontists can measure:
- Condylar volume differences between left and right sides
- Ramus height and width variations
- Maxillary width discrepancies
- Dental midline deviations relative to facial midlines
CBCT treatment planning for asymmetrical cases requires careful evaluation of growth potential and the severity of skeletal discrepancies. Young patients with significant asymmetries may benefit from growth modification therapies, while adult patients might require surgical intervention combined with orthodontic treatment.
Vertical Dimension Assessment and Open Bite Evaluation
Vertical skeletal problems present some of the most challenging cases in orthodontic treatment, and CBCT orthodontics provides unparalleled insight into these complex malocclusions. The technology allows precise measurement of anterior and posterior facial heights, helping identify the underlying skeletal causes of open bite malocclusions.
Skeletal open bite patterns often involve increased anterior facial height, steep mandibular plane angles, and altered growth patterns of the maxilla and mandible. CBCT cephalometric analysis reveals whether the open bite results from excessive maxillary vertical growth, deficient mandibular forward growth, or a combination of vertical and horizontal skeletal discrepancies.
The three-dimensional nature of cone beam computed tomography enables evaluation of the entire vertical dimension of the face, including:
- Anterior-posterior facial height ratios
- Maxillary incisor eruption patterns
- Mandibular plane angle measurements
- Condylar positioning and TMJ relationships
Orthodontic imaging through CBCT also reveals the relationship between airway dimensions and vertical facial growth. Patients with skeletal open bites frequently show constricted posterior airways, which may contribute to mouth breathing habits and perpetuate the vertical growth pattern.
Dental CBCT applications in open bite evaluation include assessment of molar eruption patterns, evaluation of posterior teeth positioning, and analysis of alveolar bone heights. The technology helps distinguish between dentoalveolar compensation and true skeletal vertical excess, which directly impacts treatment planning decisions.
CBCT orthodontic diagnosis of vertical discrepancies provides the foundation for successful treatment outcomes, whether through growth modification in younger patients or surgical orthodontic approaches in adults with severe skeletal vertical excess patterns.
Comprehensive Cephalometric Analysis Using CBCT Data

Traditional Cephalometric Measurements in Three Dimensions
CBCT orthodontics revolutionizes how practitioners perform cephalometric analysis by adding depth to traditionally flat measurements. Unlike conventional lateral cephalograms that compress three-dimensional structures into a single plane, CBCT cephalometric analysis provides true spatial relationships between skeletal landmarks.
The technology enables clinicians to measure angular and linear parameters with enhanced accuracy, eliminating the magnification errors and landmark superimposition issues common in 2D radiography. Key measurements like ANB angle, SNA, SNB, and mandibular plane angle can now be assessed in their actual anatomical positions. This precision proves particularly valuable when diagnosing skeletal Class II malocclusion cases where subtle skeletal discrepancies might be missed on traditional films.
3D dental imaging allows for the creation of custom cephalometric analyses tailored to individual patient anatomy. Practitioners can generate multiple viewing planes simultaneously, providing comprehensive assessment of anteroposterior, vertical, and transverse skeletal relationships. The ability to visualize asymmetries becomes crucial for complex cases where traditional methods fall short.
Digital workflow integration with specialized software enables automated landmark identification and measurement calculation, reducing human error while maintaining diagnostic accuracy. This technological advancement streamlines the diagnostic process while providing more reliable data for treatment planning decisions.
Soft Tissue Profile Evaluation and Planning
Modern orthodontic imaging extends beyond skeletal analysis to include detailed soft tissue assessment through CBCT data. The technology captures the complete facial profile in three dimensions, allowing practitioners to evaluate tissue thickness variations across different facial regions and predict treatment outcomes more accurately.
Soft tissue analysis becomes particularly important when planning treatments that will significantly alter facial aesthetics. CBCT data enables measurement of lip thickness, chin projection, and nasolabial angle relationships with unprecedented precision. The technology also reveals how underlying skeletal changes will translate to visible facial modifications.
Treatment simulation capabilities allow orthodontists to show patients potential outcomes before beginning therapy. This visualization tool helps set realistic expectations and improves patient compliance throughout treatment. The detailed soft tissue information also guides decisions about extraction versus non-extraction approaches and helps determine optimal anterior tooth positioning.
Airway Assessment for Sleep-Related Breathing Disorders
CBCT orthodontics provides comprehensive airway evaluation capabilities that traditional imaging methods cannot match. The technology captures the entire upper airway volume, from nasal passages through the pharyngeal spaces, enabling detailed analysis of potential breathing obstructions.
Volumetric measurements of different airway segments help identify constriction points that might contribute to sleep-disordered breathing. The technology measures minimum cross-sectional areas, total airway volumes, and identifies anatomical features that could impact airflow patterns. This information proves invaluable when planning treatments for patients with concurrent orthodontic needs and breathing disorders.
Orthodontic diagnosis technology now incorporates airway considerations as a standard component of treatment planning. Practitioners can assess how different treatment approaches might impact airway dimensions and select methods that optimize both dental alignment and respiratory function. The integration of airway analysis into routine orthodontic evaluation represents a significant advancement in comprehensive patient care.
Root Position and Bone Thickness Evaluation
Precise root positioning assessment represents one of the most significant advantages of CBCT treatment planning over traditional methods. The technology reveals exact root angulations, proximity to adjacent roots, and relationships to vital structures like the mandibular canal or maxillary sinus.
Alveolar bone thickness measurements guide treatment mechanics and help prevent complications like fenestrations or dehiscences during tooth movement. CBCT data shows bone density variations and identifies areas where careful force application becomes critical. This information proves essential when planning complex movements like intrusion, extrusion, or significant root repositioning.
Dental CBCT applications extend to impacted tooth localization and surgical planning. The technology provides precise spatial coordinates for impacted canines or other teeth, enabling minimally invasive surgical approaches and optimal orthodontic force vectors for successful eruption guidance. Root resorption monitoring also becomes more accurate with three-dimensional imaging, allowing early detection and treatment modification when necessary.
The detailed anatomical information available through CBCT imaging transforms treatment planning from educated guesswork to precision-guided therapy, resulting in more predictable outcomes and reduced treatment complications.
Treatment Planning Optimization Through CBCT Imaging
Surgical Orthodontics Case Selection and Planning
CBCT orthodontics transforms how practitioners approach complex skeletal discrepancies requiring surgical intervention. Traditional 2D radiographs often mask critical anatomical relationships, while CBCT treatment planning reveals precise spatial positioning of vital structures like the inferior alveolar nerve, maxillary sinuses, and temporomandibular joints.
The technology excels in identifying patients who truly need orthognathic surgery versus those manageable through conventional orthodontics alone. When evaluating skeletal Class II malocclusion cases, CBCT data helps distinguish between dentoalveolar compensation and genuine skeletal dysplasia. Patients with severe anteroposterior discrepancies exceeding 8mm often require surgical correction, which becomes crystal clear through volumetric analysis.
Pre-surgical planning benefits enormously from 3D dental imaging capabilities. Surgeons can visualize exact bone thickness, root positions relative to osteotomy sites, and potential complications before the first incision. Virtual surgical planning software integrates CBCT data to simulate movements, predict soft tissue changes, and optimize surgical vectors.
Post-surgical orthodontic movement also requires careful consideration of altered bone density and healing patterns. CBCT scans taken 6-8 weeks post-surgery reveal bone regeneration status and guide orthodontic reactivation timing. This precision reduces treatment time and improves stability compared to traditional guesswork approaches.
Temporary Anchorage Device Placement Precision
Mini-implant success rates dramatically improve with CBCT-guided placement protocols. Cone beam computed tomography reveals optimal insertion sites by mapping cortical bone thickness, root proximity, and anatomical landmarks with submillimeter accuracy.
Safe zones for TAD placement vary significantly between patients and anatomical regions. CBCT orthodontics data shows that interradicular spaces between maxillary premolars often provide 2-4mm of safe placement width, while mandibular posterior regions may offer less due to lingual inclination of roots. The technology identifies these variations before placement, preventing root damage and implant failure.
Angulation planning becomes surgical-level precise with volumetric imaging. Practitioners can determine optimal insertion angles to maximize cortical engagement while avoiding vital structures. Bicortical engagement, particularly in the anterior palate, shows superior retention rates when planned using CBCT data versus clinical estimation alone.
| Placement Site | Success Rate with CBCT | Success Rate without CBCT |
|---|---|---|
| Maxillary Buccal | 94% | 78% |
| Mandibular Buccal | 91% | 73% |
| Palatal | 96% | 82% |
Recovery protocols also benefit from pre-placement bone quality assessment. Dense cortical bone requires different healing timelines than trabecular bone, information clearly visible on CBCT scans but impossible to determine clinically.
Extraction Versus Non-Extraction Decision Making
Orthodontic diagnosis technology reaches new heights when addressing extraction decisions through comprehensive CBCT analysis. Traditional methods rely heavily on dental models and 2D cephalometric norms, often missing crucial three-dimensional relationships that influence long-term stability.
Crowding assessment becomes far more accurate when practitioners evaluate actual available space versus required space using volumetric measurements. CBCT reveals true arch width potential by measuring basal bone dimensions rather than estimating from dental positions. Cases showing less than 4mm of basal bone deficiency often respond well to expansion, while greater discrepancies typically require extractions.
Airway considerations play increasingly important roles in extraction planning. CBCT cephalometric analysis reveals how tooth movement affects pharyngeal dimensions and tongue positioning. Non-extraction approaches that advance the dentition often improve airway volume, while extraction treatments may compromise breathing space in susceptible patients.
Profile changes become predictable through soft tissue analysis integrated with hard tissue movements. The technology shows how lip support changes with incisor retraction, helping practitioners balance facial esthetics with dental function. Patients with thin lip morphology often benefit from non-extraction approaches to maintain facial fullness.
Periodontal considerations emerge clearly through bone thickness measurements around individual teeth. Thin buccal plates, particularly common in mandibular incisors, may indicate higher risk for recession with extensive tooth movement, favoring strategic extractions over aggressive alignment attempts.
Clinical Workflow Integration and Patient Benefits
Reduced treatment time through accurate diagnosis
CBCT orthodontics revolutionizes diagnostic precision by providing three-dimensional visualization that traditional 2D imaging simply can’t match. When orthodontists can see exactly how skeletal structures relate to each other in all dimensions, they make faster, more confident treatment decisions. This accuracy eliminates the guesswork that often leads to mid-treatment adjustments and course corrections.
The detailed anatomical information from cone beam computed tomography allows practitioners to identify skeletal malocclusion patterns immediately, rather than discovering complications months into treatment. Root positioning, bone density variations, and anatomical anomalies become visible from day one, preventing the trial-and-error approach that extends treatment timelines. Patients benefit from streamlined care that gets them to their final result more efficiently.
Improved patient communication with 3D visualization
3D dental imaging transforms how orthodontists explain complex skeletal conditions to their patients. Instead of pointing at confusing 2D radiographs and asking patients to imagine spatial relationships, practitioners can rotate and manipulate CBCT images to show exactly what’s happening inside the mouth and jaw.
Parents of children with skeletal Class II malocclusion can see precisely why their child needs specific treatment approaches. The visual evidence makes treatment recommendations more compelling and helps patients understand the value of comprehensive care. This enhanced communication builds stronger doctor-patient relationships and increases treatment acceptance rates. Patients feel more confident about their investment when they can literally see what needs correction.
Enhanced interdisciplinary collaboration capabilities
CBCT treatment planning creates a common language between orthodontists, oral surgeons, periodontists, and other specialists. The shared 3D dataset allows each practitioner to evaluate the same anatomical structures from their specialty perspective, leading to more coordinated care plans.
Surgical orthodontics cases particularly benefit from this collaborative approach. The orthodontist can plan tooth movements while the surgeon simultaneously evaluates bone structure and surgical access. This coordination prevents conflicts between treatment phases and ensures each specialist’s work supports the overall treatment goals. Digital file sharing makes consultation more efficient, reducing the time patients wait between appointments and specialist referrals.
Long-term stability prediction and monitoring
CBCT cephalometric analysis provides baseline measurements that help predict treatment stability over time. The comprehensive bone and tooth position data allows orthodontists to identify factors that might contribute to relapse, such as unfavorable growth patterns or anatomical constraints.
Post-treatment monitoring becomes more precise when practitioners can compare detailed before-and-after images. Small changes in tooth position or skeletal relationships that might indicate the beginning of relapse show up clearly in follow-up scans. This early detection allows for minor adjustments that prevent major retreatment needs. The investment in initial CBCT imaging often pays dividends in long-term treatment stability.
Minimized treatment complications and revisions
Orthodontic imaging technology helps identify potential complications before they occur. Root resorption risks, impacted teeth, and anatomical variations that could interfere with planned tooth movements become apparent during initial CBCT evaluation. This foresight allows orthodontists to modify treatment plans proactively rather than reactively.
The precise measurements from dental CBCT applications also reduce the likelihood of overcorrection or undercorrection. When practitioners know exactly how much space is available and how teeth can move within existing bone structure, they can plan more conservative, predictable movements. This precision reduces the need for treatment revisions and additional procedures that extend overall treatment time and cost for patients.
CBCT technology has revolutionized how orthodontists diagnose and treat skeletal malocclusions. From detailed three-dimensional imaging to precise cephalometric measurements, this advanced diagnostic tool gives clinicians the complete picture they need for accurate treatment planning. The ability to visualize complex skeletal patterns in 3D means better outcomes for patients and more predictable results for practitioners.
Integrating CBCT into your clinical workflow doesn’t just improve diagnostic accuracy – it transforms the entire patient experience. When you can show patients exactly what’s happening with their bite and jaw alignment, treatment discussions become clearer and more collaborative. The investment in CBCT technology pays dividends through enhanced treatment precision, reduced chair time, and ultimately, happier patients who understand and trust their treatment plan.
